What is an Infantile Hemangioma?
Infantile hemangiomas are benign vascular tumors of childhood, characterized by endothelial cell proliferation. They are the most common soft-tissue tumors of childhood, occurring in 3% to 10% of the population. The lesions are usually not detectable at birth but appear during the first 4 to 6 weeks of life. All infantile hemangiomas exhibit characteristic evolution with early rapid growth (proliferation) followed by a stabilization period and a slow spontaneous involution. The growth phase can extend up to 6 months of age, followed by an involution phase over a period of 3 to 7 years.
Although most are not worrisome, around 12% of infantile hemangiomas are significantly complex; requiring referral to specialists for consideration of treatment.
Known risk factors for the development of infantile hemangiomas are: females (female to male ratio of 2.4:1), Caucasians, low birth weight, and children of multiple gestations.
The causes of infantile hemangiomas are not well understood. The tumor is formed from the proliferation of the endothelial cells. Studies suggest the role of fetal hypoxic stress as the triggering signal that initiates the proliferation and abnormal blood vessel formation through activation of certain genes. Incomplete vasculature maturation and maternal chorionic-villus sampling has also been suggested as a potential cause of hemangiomas. Placental and infantile hemangioma cells have similar cell markers which supports the theory of IH representing “benign metastases” originating from placenta. Endothelial progenitor cells (EPCs) are vascular stem cells that are now believed to play a role in the etiology of IH; they are increased 15-fold as compared to controls.
Please consult your doctor if your child develops a birthmark that grows rapidly. They can help you understand your child’s condition more thoroughly.
Typical features of IH at birth are the appearance of a small red or white mark or bruise. While hemangiomas can appear anywhere on the body, the majority of IH cases are seen on the head and neck. Many hemangiomas are not harmful. However, during the growth stage, a hemangioma can affect vital functions depending on its location on the child’s body. It can also cause bleeding or break down of the layer of skin over the hemangioma. Since other complications may arise, it is important to ask your doctor what signs to look for to help avoid serious health problems.
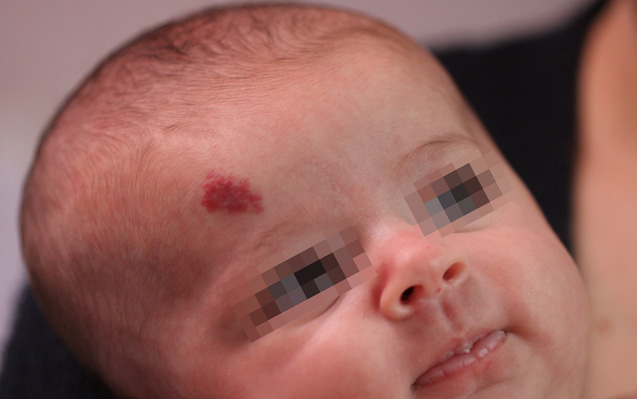
Nacent Hemangioma
Two types of hemangiomas
There are two basic types of hemangiomas: infantile hemangioma and congenital hemangioma.
Infantile hemangiomas are usually not present at birth and they start growing after birth. They look red and grow rapidly. They can be divided into:
- Superficial Hemangiomas (50-60%) often described as “strawberry” hemangiomas present as bright red tumors.
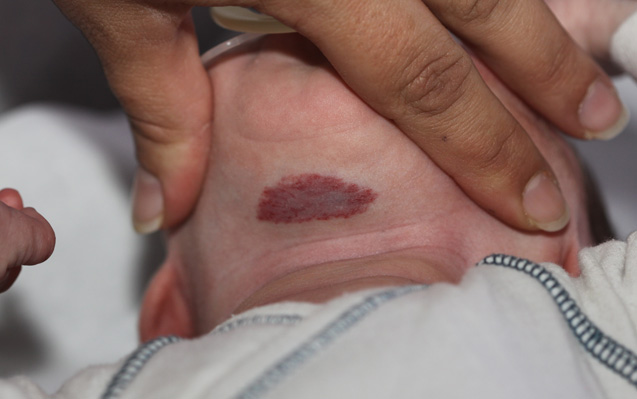
Superficial Hemangioma
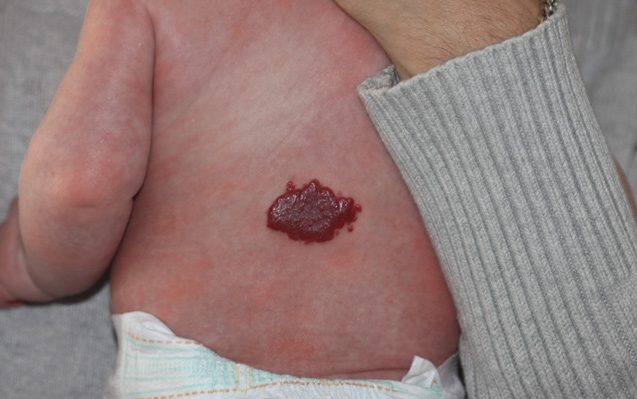
Superficial Hemangioma
- Deep Hemangiomas (15%) present as protruding tumors that are below the skin which appears normal or bluish color.
- Mixed Hemangiomas (25-35%) are a combination of both components, superficial and deep.
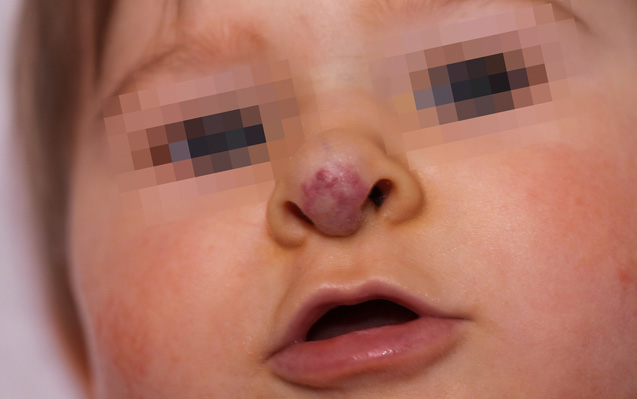
Mixed Hemangioma
Three out of four IHs belong to the nodular type. These lesions are discrete and oval or round; they are not typically associated with malformations.
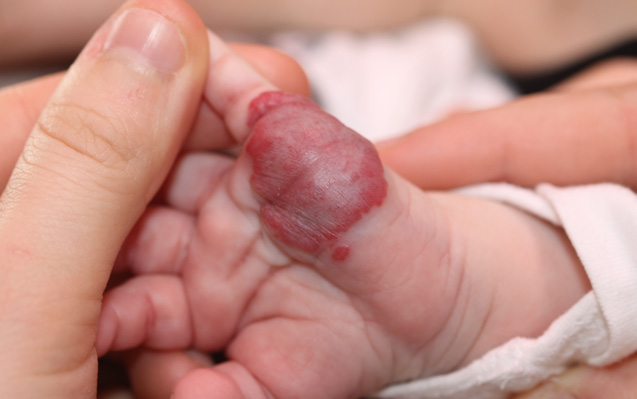
Nodular Hemangioma
Nodular hemangioma is the most common form.
Segmental hemangiomas extend across a large anatomical region and have a geographical shape; they are typically at higher risk of complications and may be associated with developmental abnormalities. Infantile hemangiomas can also belong to indetermined and multifocal type.
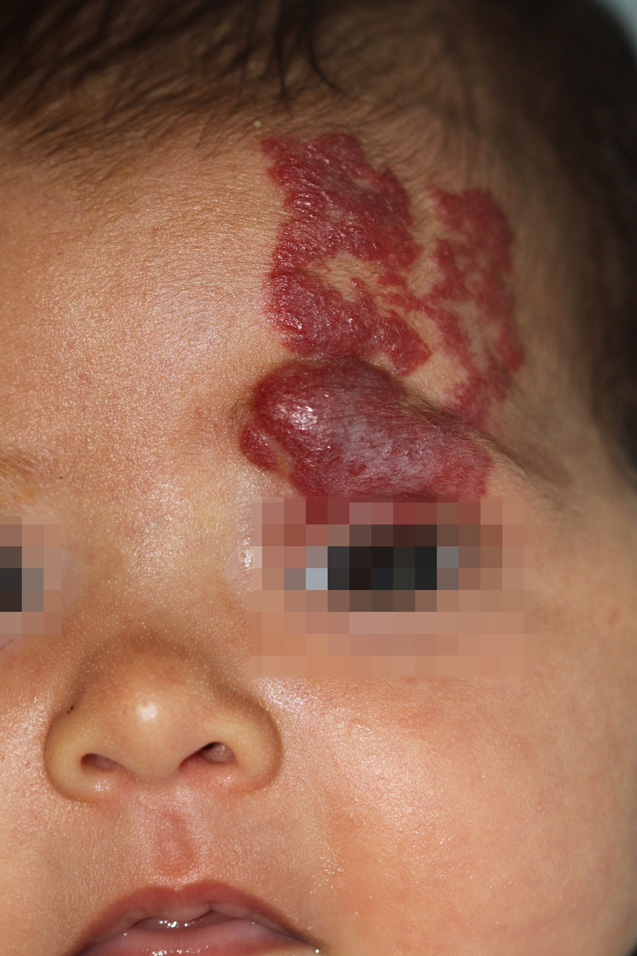
Segmental Hemangioma
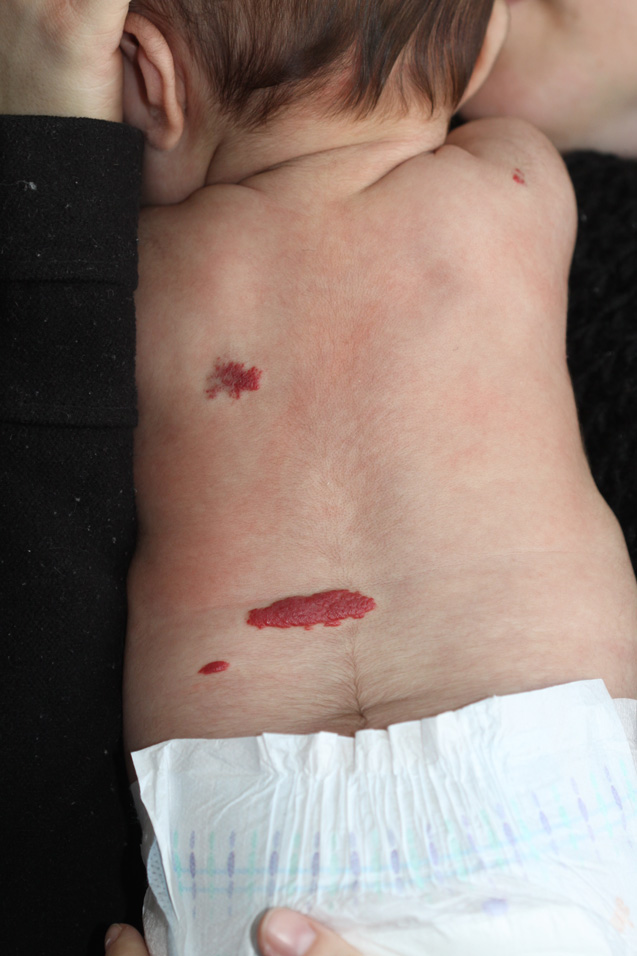
Multifocal Hemangioma
Your child’s doctor can explain what type of hemangioma your child has.
Congenital hemangiomas are vascular lesions that can be detected by prenatal ultrasounds. They develop intrauterinely and are present at birth, they appear round or oval, and vary in color from a pink to purple. The affected skin is usually raised and warm to touch.
Diagnostic differentiation can be made by histologically identifying GLUT-1 marker in infantile hemangiomas. Congenital hemangiomas are GLUT-1 negative. There are two types of congenital hemangiomas : RICH type, fully developed at birth and rapidly involuting during the first year of life. NICH type is also present at birth and it does not change during life.
Antaya RJ. Infantile hemangioma. 2007;1-20.
Hemangiomas. Arkansas Children’s Hospital Web site. Accessed January 21, 2013. Visit website »
Ballah D, Cahill AM, Fontalvo L, et al. Vascular anomalies: what they are, how to diagnose them, and how to treat them. Curr Probl Diagn Radiol. 2011;40:233-247.
Bauland CG, Lüning TH, Smit JM, Zeebregts CJ, Spauwen PHM. Untreated hemangiomas: growth pattern and residual lesions. Plast Reconstr Surg. 2011;127:1643-1648.
Boye E, Yu Y, Paranya G, et al. Clonality and altered behavior of endothelial cells from hemangiomas. J Clin. Invest. 2001;107:745-752.
Chen TS, Eichenfield LF, Friedlander SF. Infantile hemangiomas: an update on pathogenesis and therapy. Pediatrics. 2013;131:99-108.
Chiller KG, Passaro D, Frieden IJ. Hemangiomas of infancy. Clinical characteristics, morphologic subtypes, and their relationship to race, ethnicity, and sex. Arch Dermatol. 2002;138:1567-1576.
Enjolras O, Wassef M, Chapot R. Introduction: ISSVA classification. In: Editor’s name, ed. Color Atlas of Vascular Tumors and Vascular Malformations. City, State of publication: Cambridge University Press; 2007:2-11 (page numbers).
Enjolras O, Mulliken JB. Vascular tumors and vascular malformations (new issues). Adv Dermatol. 1998;13:375-423.
Haggstrom AN, Drolet BA, Baselga E, et al. Prospective study of infantile hemangiomas: demographic, prenatal, and perinatal characteristics. J Pediatr. 2007;150:291-294.
Kleinman ME, Greives MR, Churgin SS, et al. Hypoxia-induced mediators of stem/progenitor cell trafficking are increased in children with hemangioma. Arterioscler Thromb Vasc Biol. 2007;27;2664-2670.
Léauté-Labrèze C,Prey S, Ezzedine K. Infantile haemangioma: Part I. Pathophysiology, epidemiology, clinical features, life cycle and associated structural abnormalities. JEADV. 2011;1-9. [epub ahead of print]
Martin K, Bleib F, Chamlin SL, et al. Propranol treatment of infantile hemangiomas: anticipatory guidance for parents and caretakers. Pediatr Dermatol. 2013;30(1):155-159.
North PE, Waner M, Mizeracki A, Mihm MC. GLUT1: a newly discovered immunohistochemical marker for juvenile hemangiomas. Hum Pathol. 2000;31(1):11-22.
Birthmarks and vascular anomalies center infantile hemangiomas. University of California, San Francisco School of Medicine Web site. Department of Dermatology. Accessed January 17, 2013. Visit website »
van Steensel MAM. Infantile hemangiomas how to know when they grow. Arch Dermatol. 2008;144(12):1650-1650.




